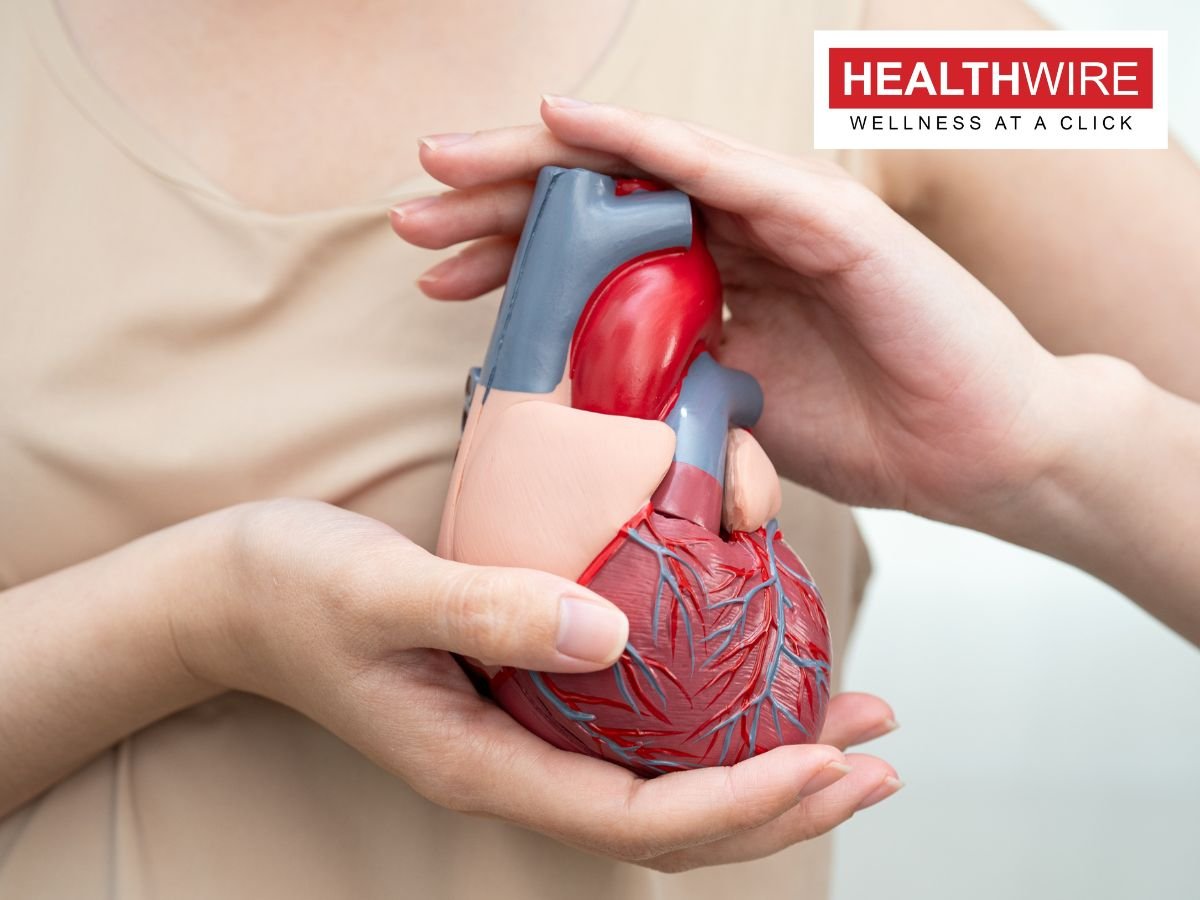
Heart disease is often perceived as a condition that primarily affects men, but it is the leading cause of death among women globally. What makes it particularly dangerous in women is that symptoms can be subtle, atypical, or even “silent,” leading to delayed diagnosis and treatment. Understanding these signs can be life-saving.
Why Heart Disease Can Be Silent in Women
Women’s heart disease often differs from men’s in both presentation and progression. While men may experience the classic symptom of severe chest pain during a heart attack, women may have less obvious warning signs. Hormonal differences, smaller coronary arteries, and variations in plaque formation contribute to these atypical symptoms, making early detection more challenging.
Commonly Missed Symptoms
Recognising heart disease early is crucial. Women should be aware of symptoms that are frequently overlooked:
- Shortness of breath: Feeling unusually breathless during routine activities or at rest may indicate underlying heart problems.
- Fatigue: Persistent exhaustion that does not improve with rest can be a subtle sign of cardiac stress.
- Nausea or indigestion: Some women report digestive discomfort, bloating, or nausea instead of chest pain.
- Pain in unusual areas: Discomfort may appear in the neck, jaw, shoulder, upper back, or abdomen.
- Dizziness or lightheadedness: Feeling faint or weak can signal inadequate blood flow to the heart.
- Palpitations or irregular heartbeat: Awareness of rapid or irregular heartbeats may indicate arrhythmia.
These symptoms are often mistaken for stress, fatigue, or gastrointestinal issues, which can delay medical attention.
Risk Factors Specific to Women
Several factors increase a woman’s risk of heart disease:
- Menopause and hormonal changes: Reduced estrogen levels can affect blood vessels and cholesterol.
- Diabetes: Women with diabetes are at a higher risk of developing heart disease than men with the same condition.
- Obesity and sedentary lifestyle: Excess weight, poor diet, and inactivity contribute to cardiovascular risk.
- High blood pressure and cholesterol: Uncontrolled hypertension or dyslipidemia accelerates arterial damage.
- Family history: Genetics can significantly influence heart disease susceptibility.
Awareness of these risk factors can prompt earlier screening and preventive measures.
Importance of Early Detection
Early detection of heart disease can prevent serious complications such as heart attacks, heart failure, and sudden cardiac death. Women should discuss regular cardiovascular screenings with their healthcare providers, especially if they have risk factors. Tests may include blood pressure monitoring, cholesterol checks, ECGs, echocardiograms, or stress tests.
Lifestyle Changes That Reduce Risk
Preventive strategies are highly effective in lowering heart disease risk:
- Healthy diet: Emphasize fruits, vegetables, whole grains, lean proteins, and healthy fats.
- Regular physical activity: Aim for at least 150 minutes of moderate-intensity exercise per week.
- Maintain a healthy weight: Weight management reduces strain on the heart and arteries.
- Avoid tobacco and limit alcohol: Smoking and excessive drinking accelerate cardiovascular damage.
- Stress management: Mindfulness, yoga, and adequate rest support heart health.
Combining lifestyle interventions with routine medical care improves outcomes significantly.
Women should consult a doctor if they experience persistent fatigue, unexplained shortness of breath, or unusual chest discomfort. Even mild or intermittent symptoms should not be ignored. Early evaluation can save lives by identifying hidden cardiovascular problems before they escalate.
Heart disease in women is often silent but deadly. By recognising subtle symptoms, understanding personal risk factors, and prioritising preventive care, women can protect their hearts and improve long-term health. Awareness and timely action are the most powerful tools in fighting this invisible threat.