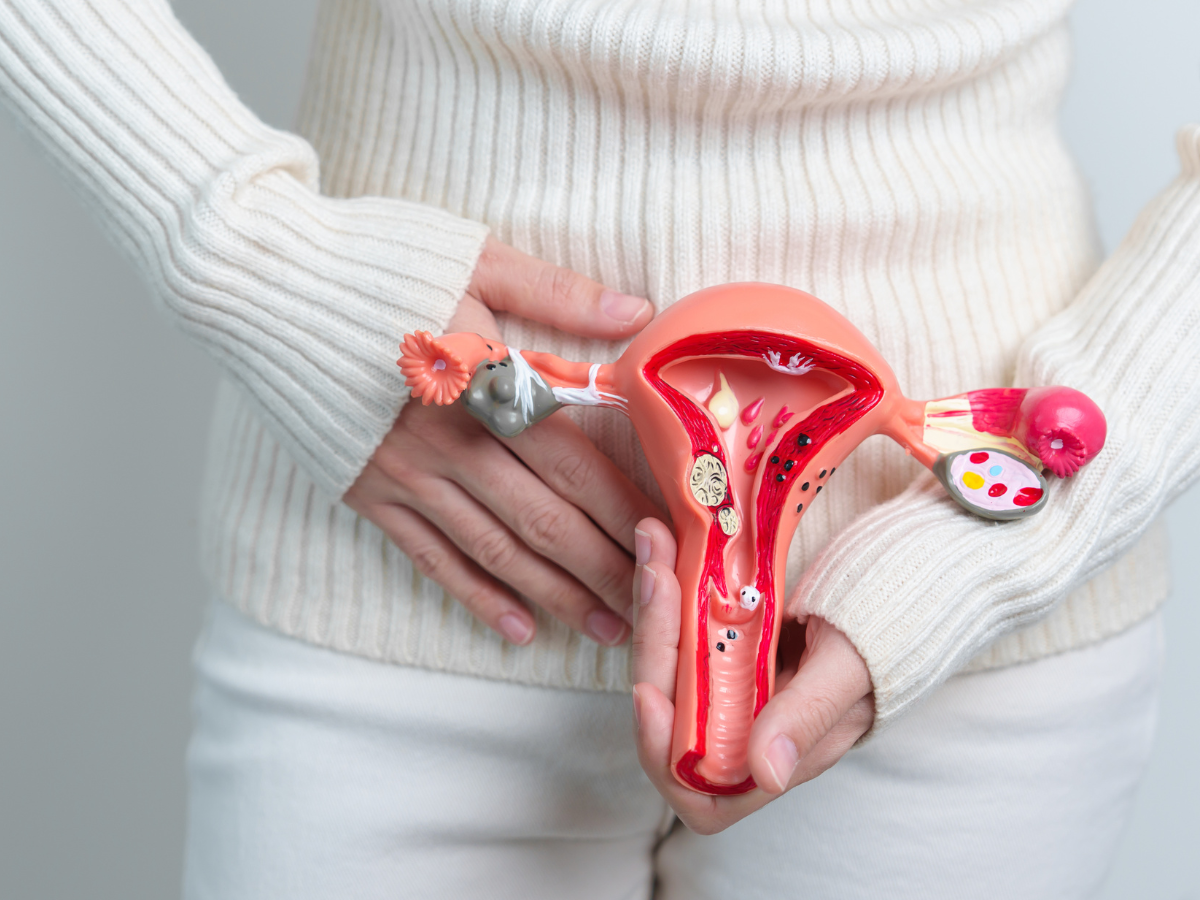
Cervical cancer remains one of the most common cancers among women in India. Early detection and timely treatment can save lives, but the costs of care can be high. While health insurance is a valuable tool to reduce financial burden, it often doesn’t cover all aspects of treatment. Understanding what is typically excluded can help patients and families plan better.
Common Coverage in Cervical Cancer Insurance
Most health insurance policies cover hospitalisation costs, including:
- Surgery for cancer removal
- Hospital room and board
- Standard medications administered during inpatient care
- Basic diagnostics during hospitalisation
However, the coverage often ends here. Out-of-pocket expenses for many essential aspects of care can still be substantial.
Diagnostic Tests Often Excluded
Early and accurate diagnosis is critical in cervical cancer care, but insurance policies may limit or exclude advanced diagnostics, such as:
- HPV typing tests
- PET scans and advanced imaging for staging
- Genetic and molecular testing
- Biopsies outside of hospital admission
Patients may need to pay for these tests separately, even though they are vital for treatment planning.
Outpatient and Follow-Up Care
Insurance often focuses on hospitalisation, leaving outpatient care largely uncovered. This includes:
- Follow-up consultations with oncologists or specialists
- Chemotherapy or targeted therapy administered on an outpatient basis
- Radiation therapy sessions outside the hospital stay
- Routine blood tests and scans for monitoring response to treatment
Since cervical cancer treatment usually involves multiple cycles of therapy over months, these expenses can add up quickly.
Medications and Supportive Therapy
While some drugs administered during hospitalisation may be covered, insurance often excludes:
- Oral chemotherapy or targeted therapy taken at home
- Pain management medications and supportive drugs
- Hormonal therapy and immunotherapy not listed in the policy
- Supplements and nutrition therapy to manage treatment side effects
Patients should carefully review their policy to know which medications are reimbursable.
Lifestyle and Auxiliary Costs
Cervical cancer care often involves additional non-medical costs that insurance usually does not cover:
- Travel and accommodation for repeated visits to specialized centres
- Counseling, mental health therapy, and support groups
- Physiotherapy or rehabilitation services
- Diet and nutrition planning specific to cancer recovery
While essential for patient well-being, these costs often fall entirely on the patient.
Insurance Limitations and Tips
Even when policies claim to cover cancer, there are common limitations:
- Capping of treatment costs: Some plans have annual or per-treatment limits.
- Waiting periods: Newly purchased policies may not cover pre-existing or recently diagnosed cancers immediately.
- Network restrictions: Coverage may be limited to certain hospitals, affecting access and convenience.
Tips for patients:
- Review your policy’s cancer coverage in detail before treatment.
- Ask the insurer about outpatient chemotherapy, targeted therapy, and supportive medications.
- Keep track of receipts and bills to maximize reimbursements.
- Consider specialized cancer insurance plans that cover diagnostics, outpatient care, and supportive therapy.
Cervical cancer treatment can be financially and emotionally taxing. While health insurance offers essential support, it often does not cover diagnostic tests, outpatient therapies, medications taken at home, or supportive care services. Awareness of these gaps allows patients and families to plan ahead, explore additional insurance options, and make informed decisions about treatment without unexpected financial stress.