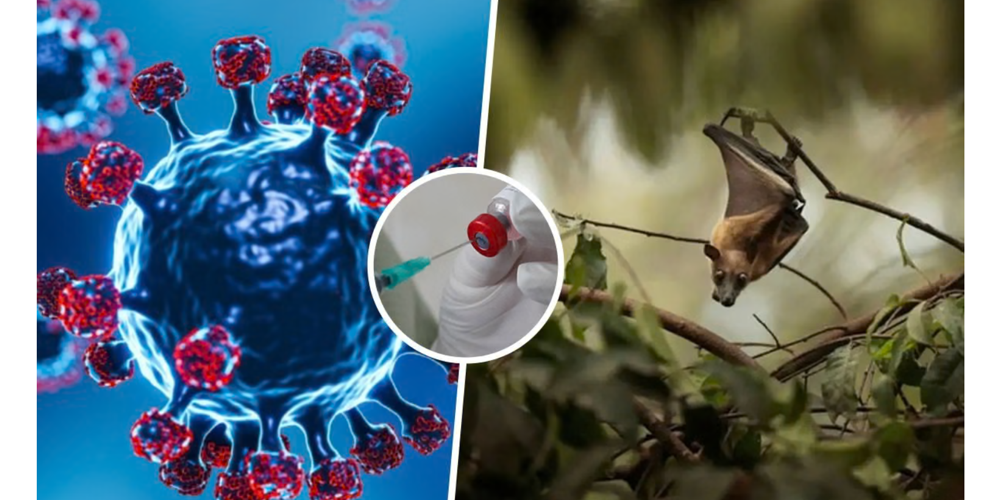
India has faced sporadic outbreaks of the Nipah virus over the past two decades, most notably in Kerala in 2001, 2018, and 2019. While each outbreak was successfully contained, the virus’s high fatality rate—ranging between 40% and 75%—continues to raise serious public health concerns. According to Dr. Dip Narayan Mukherjee, Consultant in Microbiology and Infectious Diseases at CK Birla Hospital, CMRI, India’s ability to manage future Nipah threats depends far more on preparedness and discipline than on reactive, panic-driven measures.
“Nipah is a highly lethal RNA virus, but it does not spread easily if early detection and infection control protocols are followed meticulously,” Dr. Mukherjee explains. “The key is not to underestimate early symptoms or delay isolation.”
Early Detection Remains the Cornerstone
One of the most important pillars of India’s preparedness, as highlighted by Dr. Mukherjee, is early detection. Nipah infection often begins with non-specific flu-like symptoms such as fever, headache, and body aches, which can easily be mistaken for common viral illnesses.
“What worries clinicians is not the virus itself, but the possibility of delayed diagnosis,” says Dr. Mukherjee. “Once neurological symptoms like confusion, altered sensorium, or seizures appear, the disease may already be advanced. That is why every unexplained respiratory illness must be treated as a suspected case until ruled out.”
Government-issued guidelines have clearly outlined protocols for identifying and managing suspected Nipah cases. Hospitals have been advised to isolate patients immediately upon suspicion, even before laboratory confirmation, a step that has proven critical in preventing secondary transmission.
Infection Control in Hospitals: A Non-Negotiable Measure
Human-to-human transmission of Nipah virus has been documented primarily in healthcare settings. According to Dr. Dip Narayan Mukherjee, this makes infection prevention and control (IPC) measures in hospitals absolutely non-negotiable.
“Strict use of personal protective equipment—including N95 masks, gloves, gowns, and face shields—must be followed whenever a suspected case is handled,” he notes. “Barrier nursing, asepsis, and controlled patient movement are essential to protect both healthcare workers and other patients.”
India’s hospitals have significantly strengthened IPC practices since earlier outbreaks, particularly in high-risk regions. Regular training, mock drills, and refresher sessions for healthcare staff ensure that protocols are followed even under pressure.
Role of Clinical Vigilance and Training
Clinical vigilance is another critical factor in preparedness. Dr. Mukherjee stresses that awareness must extend beyond tertiary care centres to primary and secondary healthcare facilities, where patients often present first.
“A doctor in a small clinic may be the first to see a Nipah patient,” he says. “If that clinician fails to recognise the warning signs or delays referral, the risk of transmission increases.”
Training healthcare workers to recognise early red flags—especially neurological symptoms associated with respiratory illness—is crucial. Timely sample collection and referral to designated laboratories allow for faster diagnosis and containment.
Laboratory and Surveillance Readiness
India’s laboratory network plays a central role in outbreak control. According to Dr. Mukherjee, the ability to safely test samples in high-containment laboratories ensures accurate diagnosis without exposing laboratory personnel.
“Laboratory confirmation helps guide public health action,” he explains. “Once a case is confirmed, contact tracing, quarantine, and surveillance can be implemented in a focused and effective manner.”
Surveillance systems that monitor clusters of unusual respiratory or neurological illness further strengthen preparedness. Integration of clinical, laboratory, and epidemiological data allows health authorities to respond swiftly.
Community Awareness and Public Health Response
Preparedness does not stop at hospital doors. Community awareness is equally important, particularly in regions where Nipah cases have been reported in the past. Dr. Mukherjee emphasises that educating the public helps prevent fear-driven behaviour and misinformation.
“People need to know how Nipah spreads and what precautions to take, without creating unnecessary panic,” he says. “Simple measures like avoiding consumption of fruits contaminated by bats and reporting symptoms early can make a significant difference.”
Rapid response teams trained in contact tracing and risk communication have proven effective in previous outbreaks, ensuring swift containment while maintaining public trust.
Learning From Past Outbreaks
India’s experience with earlier Nipah outbreaks has significantly shaped its preparedness framework. Dr. Mukherjee points out that Kerala’s success in containing outbreaks offers valuable lessons for the rest of the country.
“The reason outbreaks did not escalate into widespread transmission was disciplined isolation, strict infection control, and transparent communication,” he explains. “Preparedness is about consistency, not crisis management.”
Remaining Challenges and the Way Forward
Despite progress, challenges remain. According to Dr. Mukherjee, awareness can decline during long gaps between outbreaks, and infrastructure varies across regions.
“Nipah is rare, which makes it easy for vigilance to drop,” he warns. “Continuous training, adequate PPE stockpiles, and strong referral systems are essential to stay ready.”
The absence of a licensed vaccine or specific antiviral treatment further underscores the importance of prevention. Until medical countermeasures become available, early detection and isolation remain the most effective tools.
Protecting Healthcare Workers
Healthcare workers are at the frontline of any Nipah response. Dr. Mukherjee stresses that their protection must remain a priority.
“If healthcare workers are not safe, the system collapses,” he says. “Ensuring proper PPE, training, and psychological support is as important as treating patients.”
In conclusion, Dr. Dip Narayan Mukherjee believes that India is reasonably well-prepared to manage future Nipah outbreaks—provided protocols continue to be followed rigorously.
“Nipah is dangerous, but it is not uncontrollable,” he concludes. “With early detection, rapid isolation, and strict infection control, we can prevent widespread transmission. Preparedness, not panic, is our strongest defence.”