The Nipah virus (NiV) is one of the deadliest zoonotic viruses known to humans. Though outbreaks are relatively rare, the virus has repeatedly raised global alarm because of its extremely high fatality rate, ability to spread from animals to humans and between humans, and the absence of a specific cure or licensed vaccine. First identified in the late 1990s, Nipah continues to resurface in South and Southeast Asia, particularly in India and Bangladesh, posing a serious public health threat.
This explainer breaks down everything you need to know about the Nipah virus—what it is, where it comes from, how it spreads, its symptoms, how deadly it is, how it is diagnosed and treated, and whether it has the potential to cause another pandemic.
What Is the Nipah Virus (NiV)?
The Nipah virus is a zoonotic virus, meaning it spreads from animals to humans. It belongs to the Henipavirus genus in the Paramyxoviridae family, the same family that includes measles and mumps viruses.
Nipah is classified as a Biosafety Level-4 (BSL-4) pathogen, the highest risk category reserved for the world’s most dangerous viruses. This classification reflects its high mortality rate, lack of targeted treatment, and potential for widespread outbreaks.
Why Is Nipah Virus Considered So Dangerous?
Several factors make Nipah virus particularly alarming:
- High fatality rate: Death rates range from 40% to 75%, depending on the outbreak and healthcare response.
- No specific treatment or vaccine currently approved for public use.
- Human-to-human transmission, especially in healthcare and family settings.
- Severe brain involvement, leading to encephalitis (brain inflammation).
- Potential for mutation, which could increase transmissibility.
Because of these risks, the World Health Organization (WHO) lists Nipah virus as a priority pathogen requiring urgent research and preparedness.
Where Did the Nipah Virus Originate?
The Nipah virus was first identified in 1998–1999 during an outbreak in Malaysia and Singapore. The outbreak affected pig farmers and slaughterhouse workers, with pigs acting as intermediate hosts.
The virus gets its name from Sungai Nipah, a village in Malaysia where the first cases were recorded.
Natural Reservoir: Where Does Nipah Virus Live?
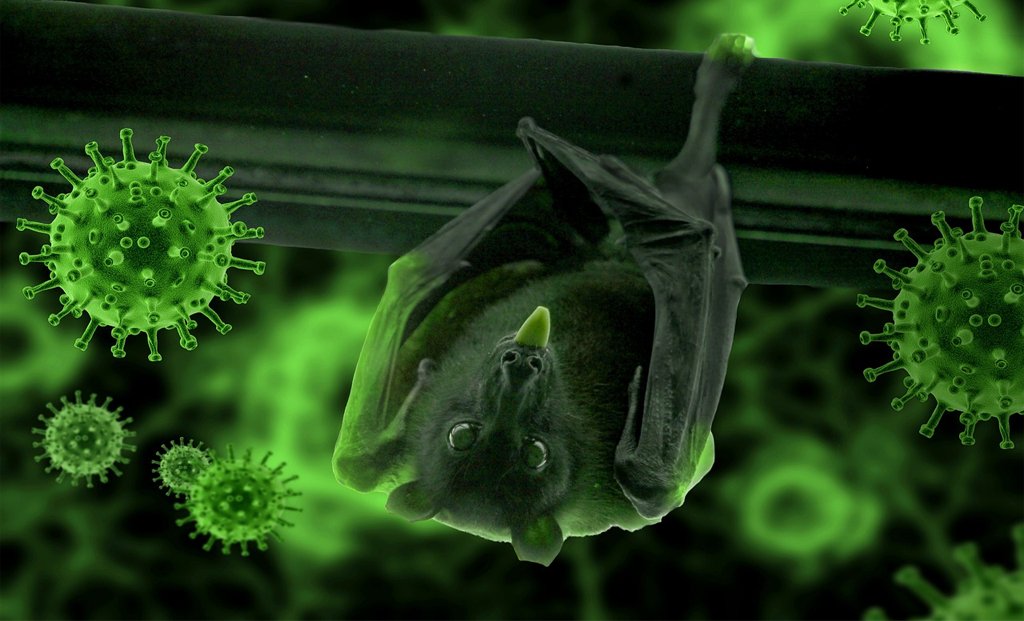
The natural hosts of Nipah virus are fruit bats, specifically bats of the Pteropus genus, commonly known as flying foxes. These bats carry the virus without falling ill and shed it through:
- Saliva
- Urine
- Feces
Fruit bats are widely distributed across South and Southeast Asia, which explains why Nipah outbreaks tend to recur in this region.
How Does Nipah Virus Spread?
Nipah virus spreads through multiple pathways, making it difficult to control.
1. Animal-to-Human Transmission
Humans can get infected by:
- Consuming raw date palm sap contaminated by bat saliva or urine
- Eating fruits partially eaten or contaminated by bats
- Direct contact with infected animals such as pigs
2. Human-to-Human Transmission
This is one of the most dangerous aspects of Nipah virus.
- Spread occurs through close contact with infected persons
- Exposure to body fluids such as saliva, urine, blood, or respiratory secretions
- Common in family caregivers and healthcare workers
3. Healthcare-Associated Transmission
Hospitals can become hotspots if:
- Infection control practices are weak
- Personal protective equipment (PPE) is inadequate
Nipah Virus in India: A Recurring Threat
India has experienced multiple Nipah outbreaks, primarily in Kerala and West Bengal.
Major Indian Outbreaks
- 2001 & 2007 – West Bengal: High fatality rates, limited awareness
- 2018 – Kerala: One of the deadliest outbreaks; fatality rate over 85%
- 2019, 2021, 2023, 2024 – Kerala: Prompt surveillance helped limit spread
Kerala’s strong public health response, contact tracing, and isolation measures have been crucial in containing recent outbreaks.
Incubation Period: How Long Before Symptoms Appear?
The incubation period of Nipah virus typically ranges from 4 to 14 days, but in some cases, it can extend up to 45 days. This long incubation period makes tracking and controlling outbreaks challenging.
Symptoms of Nipah Virus Infection
Symptoms can vary from mild to extremely severe and may progress rapidly.
Early Symptoms
- Fever
- Headache
- Muscle pain
- Sore throat
- Fatigue
- Vomiting
These early signs often resemble common viral infections, making early diagnosis difficult.
Severe Symptoms
- Acute encephalitis (brain inflammation)
- Dizziness and confusion
- Disorientation
- Seizures
- Loss of consciousness
- ComaRespiratory Symptoms
Some patients develop:
- Cough
- Shortness of breath
- Acute respiratory distress
This increases the risk of human-to-human transmission.
Long-Term Effects in Survivors
Even among survivors, Nipah virus can cause lasting complications, including:
- Persistent neurological problems
- Memory loss
- Personality changes
- Seizure disorders
In rare cases, relapsing encephalitis can occur months or even years after recovery.
How Deadly Is Nipah Virus?
The case fatality rate (CFR) of Nipah virus ranges between 40% and 75%, making it far deadlier than many well-known viruses.
- COVID-19 global fatality rate: ~1–2%
- Ebola fatality rate: ~50%
- Nipah fatality rate: up to 75%
Death often occurs due to severe brain swelling, respiratory failure, or multi-organ dysfunction.
Diagnosis: How Is Nipah Virus Detected?
Early diagnosis is critical but challenging.
Laboratory Tests
- RT-PCR (real-time polymerase chain reaction)
- ELISA tests to detect antibodies
- Virus isolation (high-security labs only)
Samples are taken from:
- Throat and nasal swabs
- Blood
- Urine
- Cerebrospinal fluid
Because Nipah requires BSL-4 labs, testing capacity is limited.
Is There a Treatment for Nipah Virus?
There is no specific antiviral treatment approved for Nipah virus.
Current Medical Care
Treatment is supportive, focusing on:
- Managing fever and pain
- Treating respiratory distress
- Controlling seizures
- Reducing brain swelling
Experimental Therapies
- Antiviral drugs like Ribavirin have been used experimentally
- Monoclonal antibodies are under research
None are yet proven as definitive cures.
Is There a Vaccine for Nipah Virus?
As of now, no licensed vaccine exists for Nipah virus.
However:
- Several vaccine candidates are in preclinical and early clinical stages
- Research is ongoing in India, the US, and Australia
- WHO has prioritized Nipah for accelerated vaccine development
How Can Nipah Virus Be Prevented?
Prevention relies heavily on behavioral and public health measures.
Individual-Level Prevention
- Avoid consuming raw date palm sap
- Wash fruits thoroughly
- Avoid fruits bitten by bats
- Avoid contact with sick animals
Community-Level Measures
- Surveillance of bat populations
- Safe farming and animal handling practices
- Public awareness campaigns
Hospital-Level Measures
- Strict infection control
- Use of PPE
- Isolation of suspected cases
Why Nipah Virus Has Pandemic Potential
Nipah virus has not yet caused a global pandemic, but experts remain concerned because:
- It spreads through respiratory droplets in close contact
- Urban outbreaks could escalate quickly
- High mutation potential
- Global travel could facilitate spread
If Nipah were to mutate into a more easily transmissible form, it could pose a serious global threat.
How Nipah Virus Is Different From COVID-19
| Feature | Nipah Virus | COVID-19 |
|---|---|---|
| Fatality rate | 40–75% | ~1–2% |
| Transmission | Close contact | Airborne |
| Vaccine | No | Yes |
| Frequency | Rare outbreaks | Global pandemic |
Nipah is deadlier but less contagious—so far.
Why Surveillance and Early Detection Matter
Quick identification, isolation, and contact tracing have proven effective in containing Nipah outbreaks, especially in Kerala. Strengthening surveillance systems is critical to prevent future escalation.
Key Takeaway: Why Nipah Virus Should Not Be Ignored
The Nipah virus may not spread as easily as some respiratory viruses, but its high fatality rate, severe neurological damage, and lack of treatment make it one of the most dangerous pathogens known today. Each outbreak is a reminder that zoonotic diseases are rising as human-animal interactions increase.
Vigilance, scientific research, public awareness, and strong healthcare systems remain the best defense against Nipah virus—before it becomes a much larger global crisis.